Lyme disease is a tick-transmitted inflammatory disorder characterized by an early focal skin lesion, and subsequently a growing red area on the skin (erythema chronicum migrans or ECM). The disorder may be followed weeks later by neurological, heart or joint abnormalities.
Symptoms
The first symptom of Lyme disease is a skin lesion. Known as erythema chronicum migrans, or ECM, this usually begins as a red 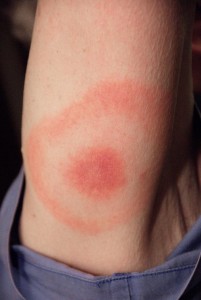 discoloration (macule) or as an elevated round spot (papule). The skin lesion usually appears on an extremity or on the trunk, especially the thigh, buttock or the under arm. This spot expands, often with central clearing, to a diameter as large as 50 cm (c. 12 in.). Approximately 25% of patients with Lyme disease report having been bitten at that site by a tiny tick 3 to 32 days before onset of ECM. The lesion may be warm to touch. Soon after onset nearly half the patients develop multiple smaller lesions without hardened centers. ECM generally lasts for a few weeks. Other types of lesions may subsequently appear during resolution. Former skin lesions may reappear faintly, sometimes before recurrent attacks of arthritis. Lesions of the mucous membranes do not occur in Lyme disease. The most common symptoms accompanying ECM, or preceding it by a few days, may include malaise, fatigue, chills, fever, headache and stiff neck. Less commonly, backache, muscle aches (myalgias), nausea, vomiting, sore throat, swollen lymph glands, and an enlarged spleen may also be present. Most symptoms are characteristically intermittent and changing, but malaise and fatigue may linger for weeks. Arthritis is present in about half of the patients with ECM, occurring within weeks to months following onset and lasting as long as 2 years. Early in the illness, migratory inflammation of many joints (polyarthritis) without joint swelling may occur. Later, longer attacks of swelling and pain in several large joints, especially the knees, typically recur for several years. The knees commonly are much more swollen than painful; they are often hot, but rarely red. Baker’s cysts (a cyst in the knee) may form and rupture. Those symptoms accompanying ECM, especially malaise, fatigue and low-grade fever, may also precede or accompany recurrent attacks of arthritis. About 10% of patients develop chronic knee involvement (i.e. unremittent for 6 months or longer). Neurological abnormalities may develop in about 15% of patients with Lyme disease within weeks to months following onset of ECM, often before arthritis occurs. These abnormalities commonly last for months, and usually resolve completely. They include:
discoloration (macule) or as an elevated round spot (papule). The skin lesion usually appears on an extremity or on the trunk, especially the thigh, buttock or the under arm. This spot expands, often with central clearing, to a diameter as large as 50 cm (c. 12 in.). Approximately 25% of patients with Lyme disease report having been bitten at that site by a tiny tick 3 to 32 days before onset of ECM. The lesion may be warm to touch. Soon after onset nearly half the patients develop multiple smaller lesions without hardened centers. ECM generally lasts for a few weeks. Other types of lesions may subsequently appear during resolution. Former skin lesions may reappear faintly, sometimes before recurrent attacks of arthritis. Lesions of the mucous membranes do not occur in Lyme disease. The most common symptoms accompanying ECM, or preceding it by a few days, may include malaise, fatigue, chills, fever, headache and stiff neck. Less commonly, backache, muscle aches (myalgias), nausea, vomiting, sore throat, swollen lymph glands, and an enlarged spleen may also be present. Most symptoms are characteristically intermittent and changing, but malaise and fatigue may linger for weeks. Arthritis is present in about half of the patients with ECM, occurring within weeks to months following onset and lasting as long as 2 years. Early in the illness, migratory inflammation of many joints (polyarthritis) without joint swelling may occur. Later, longer attacks of swelling and pain in several large joints, especially the knees, typically recur for several years. The knees commonly are much more swollen than painful; they are often hot, but rarely red. Baker’s cysts (a cyst in the knee) may form and rupture. Those symptoms accompanying ECM, especially malaise, fatigue and low-grade fever, may also precede or accompany recurrent attacks of arthritis. About 10% of patients develop chronic knee involvement (i.e. unremittent for 6 months or longer). Neurological abnormalities may develop in about 15% of patients with Lyme disease within weeks to months following onset of ECM, often before arthritis occurs. These abnormalities commonly last for months, and usually resolve completely. They include:
1. lymphocytic meningitis or meningoencephalitis
2. jerky involuntary movements (chorea)
3. failure of muscle coordination due to dysfunction of the
cerebellum (cerebellar ataxia)
4. cranial neuritis including Bell’s palsy (a form of facial
paralysis)
5. motor and sensory radiculo-neuritis (symmetric weakness, pain,
strange sensations in the extremities, usually occurring first
in the legs)
6. injury to single nerves causing diminished nerve response
(mononeuritis multiplex)
7. inflammation of the spinal cord (myelitis).
Abnormalities in the heart muscle (myocardium) occur in approximately 8% of patients with Lyme disease within weeks of ECM. They may include fluctuating degrees of atrioventricular block and, less commonly, inflammation of the heart sack and heart muscle (myopericarditis) with reduced blood volume ejected from the left ventricle and an enlarged heart (cardiomegaly). When Lyme Disease is contracted during pregnancy, the fetus may or may not be adversely affected, or may contract congenital Lyme Disease. In a study of nineteen pregnant women with Lyme Disease, fourteen had normal pregnancies and normal babies. If Lyme Disease is contracted during pregnancy, possible fetal abnormalities and premature birth can occur.
Etiology
Lyme disease is caused by a spirochete bacterium (Borrelia Burgdorferi) transmitted by a small tick called Ixodes dammini. The  spirochete is probably injected into the victim’s skin or bloodstream at the time of the insect bite. After an incubation period of 3 to 32 days, the organism migrates outward in the skin, is spread through the lymphatic system or is disseminated by the blood to different body organs or other skin sites. Lyme Disease was first described in 1909 in European medical journals. The first outbreak in the United States occurred in the early 1970’s in Old lyme, Connecticut. An unusually high incidence of juvenile arthritis in the area led scientists to investigate and identify the disorder. In 1981, Dr. Willy Burgdorfer identified the bacterial spirochete organism (Borrelia Burgdorferi) which causes this disorder.
spirochete is probably injected into the victim’s skin or bloodstream at the time of the insect bite. After an incubation period of 3 to 32 days, the organism migrates outward in the skin, is spread through the lymphatic system or is disseminated by the blood to different body organs or other skin sites. Lyme Disease was first described in 1909 in European medical journals. The first outbreak in the United States occurred in the early 1970’s in Old lyme, Connecticut. An unusually high incidence of juvenile arthritis in the area led scientists to investigate and identify the disorder. In 1981, Dr. Willy Burgdorfer identified the bacterial spirochete organism (Borrelia Burgdorferi) which causes this disorder.
Affected Population
Lyme Disease occurs in wooded areas with populations of mice and deer which carry ticks, and can be contracted during any season of the year.
Related Disorders
Rheumatoid Arthritis is a disorder similar in appearance to Lymedisease. However, the pain in rheumatoid arthritis is usually more pronounced. Morning stiffness and symmetric joint swelling more commonly occur in rheumatoid arthritis, and knotty lumps under the skin may be present over bony prominences. Bony decalcification which can be prominent in Rheumatoid Arthritis is detected on X-rays. Brachial Neuritis, also known as Parsonnage-Turner Syndrome, is a common inflammation of a group of nerves that supply the arm, forearm, and hand (brachial plexus). It is characterized by severe neck pain in the area above the collarbone (supraclavicular) that may radiate down the arm and into the hand. There also may be weakness and numbness (hyperesthesia) of the fingers and hands. Although many cases have no apparent cause, this syndrome may occur following an immunization (tetanus or diptheria), surgery, or infection with Lyme Disease.
Therapies: Standard
For adults with Lyme disease the antibiotic tetracycline is the drug of choice. Penicillin V and erythromycin have also been used. In children penicillin V is recommended rather than tetracycline. Penicillin V is now recommended for neurological abnormalities. It is not yet clear whether antibiotic treatment is helpful later in the illness when arthritis is the most predominant symptom. Treatment should be started as soon as the rash appears, even before the Enzyme Linked Immunoabsorbent Assay (ELISA) test is completed. Results of this test may be inaccurate if patients have had antibiotics soon after contracting Lyme Disease, or in those who have weakened immune systems. If lyme Disease is contracted during pregnancy, careful monitoring by physicians is highly recommended to avoid possible fetal abnormalities and/or complications. For tense knee joints due to increased fluid flowing in the joint spaces (effusions), the use of crutches is often helpful. Aspiration of fluid and injection of a corticosteroid may be beneficial. If the patient with Lyme disease has marked functional limitation, excision of the membrane lining the joint (synovectomy) may be performed for chronic (6 months or more despite therapy) knee effusions, but spontaneous remission can occur after more than a year of continuous knee involvement. When Lyme Disease is contracted during pregnancy, treatment with penicillin should begin immediately to avoid the possibility of fetal abnormalities. In 1989 a new Lyme Disease antibody test, manufactured by Cambridge Biosciences Corp., was approved by the FDA. This test is being used by local laboratories throughout the nation, making tests more available to the general population. However, it is 97% specific for antibodies to Lyme disease when compared to Western blot tests, but it cannot identify the live bacteria in patients who have not yet developed the antibodies.
Therapies: Investigational
Researchers are trying to develop a test that will identify the Lyme disease bacteria in patients who have not yet developed the antibodies. This would enable doctors to diagnose Lyme disease very early in the course of the illness. This disease entry is based upon medical information available through July 1989. Since NORD’s resources are limited, it is not possible to keep every entry in the Rare Disease Database completely current and accurate. Please check with the agencies listed in the Resources section for the most current information about this disorder.
